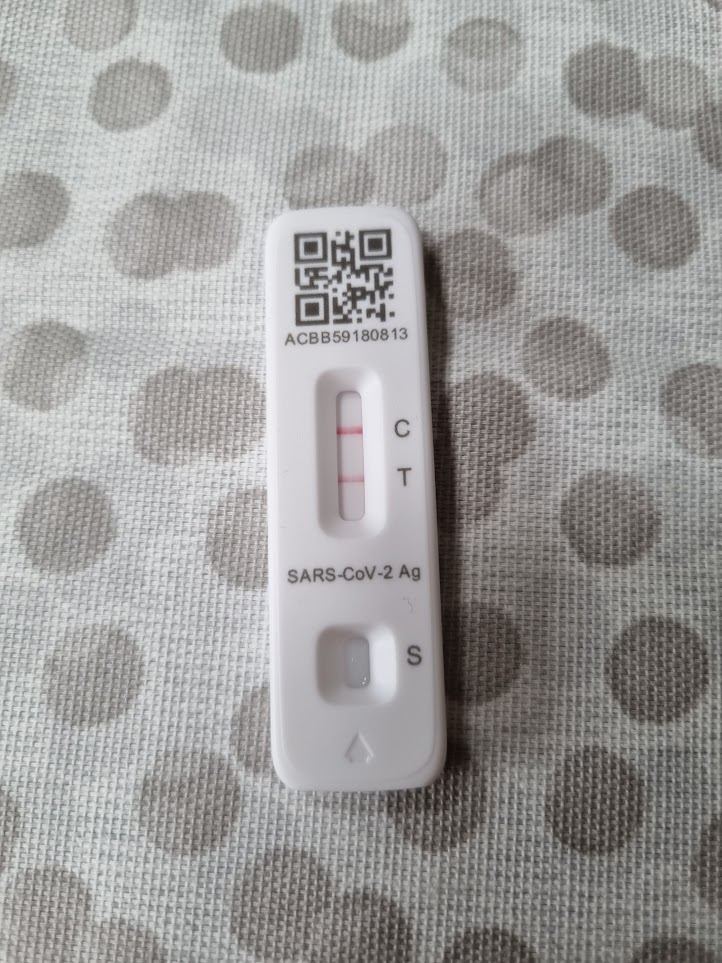
I have caught Covid for the third time this week, so naturally my thoughts have turned to how it all began.
There are a few Covid posts starting to turn up online as the 6th anniversary of it all rumbles around. The British Foreign Policy Group have helpfully published a timeline from which I have taken everything that happened before Boris Johnson locked us down for the first time:
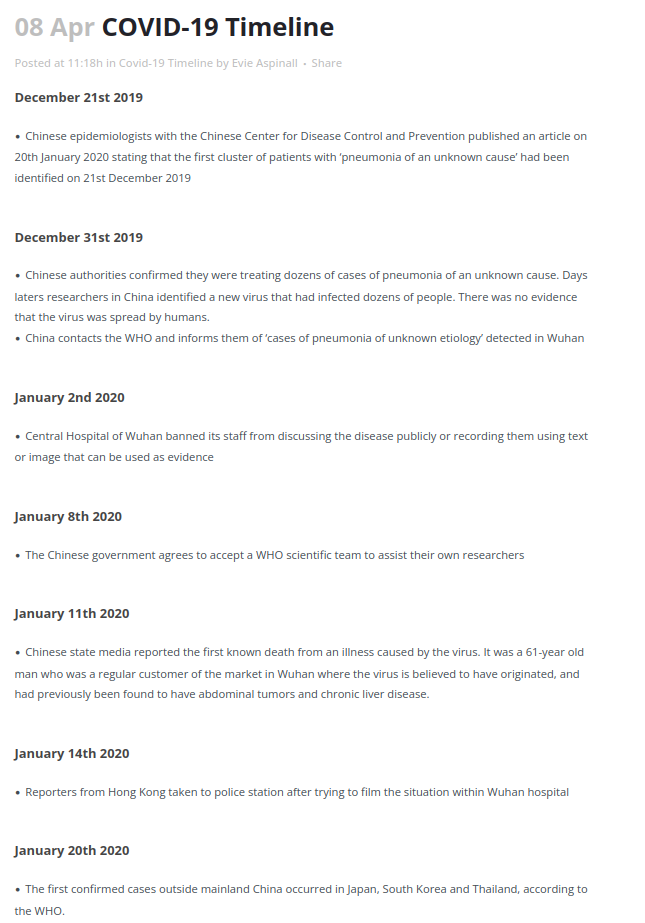

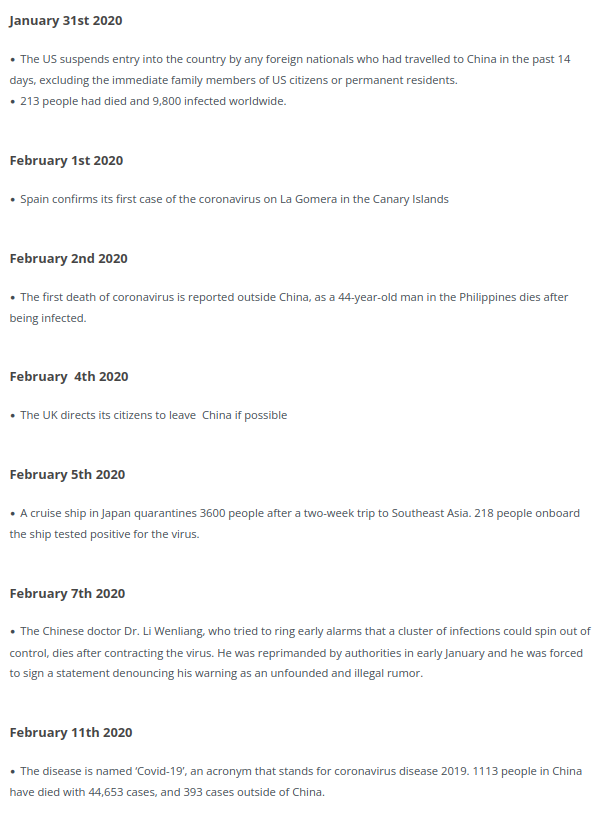




So a lot had happened by 23 March. You will all have your favourite bits from the saga above, I think mine is 22 January, when Public Health England announced they had moved the risk level to the general public from very low to low.
I remember teaching a macroeconomics class on 12 March when we knew it was going to be the last session on campus. The penny hadn’t dropped. Students were asking about how they would hand work in. We agreed it would have to be online. Some lecturers were talking about microwaving paper submissions to sterilise them. We had a little giggle about that. I had spoken to Stuart McDonald (now MBE) earlier that day where we had reluctantly agreed to postpone his visit to campus to speak to the Leicester Actuarial Science Society (LASS). Stuart would of course become one of the actuarial stars of the pandemic for his work with the COVID-19 Actuaries Response Group. I had a similar conversation by email with Lord Willetts, who was Chancellor at the University of Leicester at the time and who was going to talk to LASS about his books The Pinch and A University Education. We talked of postponing rather than cancelling. The realisation that everything was changing for the foreseeable future was still not there.
It took a long time for the penny to drop for the Government as well. As this analysis of the establishment of the “Covid Disinformation Ecosystem” says:
January featured fear and disbelief, February proved covid couldn’t simply be ignored, March was when governments realised the hospitalisation rate could overwhelm healthcare.
And a Government that was slow to respond initially was very vulnerable to the groups which sprung up during 2020 and 2021. As the Counter Disinformation Project says:
And the main initial target for the UK section of the ecosystem was Boris Johnson who was meeting privately with newspaper owners and editors. Enough doubt was put into Johnson’s mind that he dithered and delayed when cases began to rise, leading to a private meeting with Heneghan, Gupta and Sweden’s Anders Tegnell in September before he chose to ignore his scientific advisors’ calls for a circuit breaker lockdown. In the run up to the deadliest weeks of the pandemic the papers were calling for Johnson to “Save Christmas’.
However I don’t want to focus on our collective inability to make decisions during crises this time. This time I want to focus on the impact of the pandemic on our mental health.
By coincidence, today the 386 page Module 3 report from the Covid Inquiry on The impact of the Covid-19 pandemic on the healthcare systems of the United Kingdom was published. The longer this Inquiry goes on, the more it appears to resemble a truth and reconciliation commission rather than something likely to improve the handling of future pandemics. It gets past transgressions on the record, but in a way designed to move us on rather than improve our preparedness and organisation. I certainly saw nothing in the summaries that I didn’t already know. Module 3 has made 10 recommendations. The only one which mentions mental health at all is the last one on Psychological and emotional support for healthcare workers.
Looking through the module titles, it would seem that this is unlikely to be rectified until Module 10 – Impact on society – reports, currently scheduled for the first half of 2027. I find this relegation of our collective trauma to the lowest priority astonishing.
Two years ago, the Centre for Mental Health produced a review of the evidence so far on COVID-19 and the Nation’s Mental Health. They noted that:
Data on the prevalence of mental health difficulties is harder to assess. For children and young
people, surveys in England have provided a time series since 2020 that suggests very strongly that
mental ill health is indeed more prevalent now than it was before the start of the pandemic. A steady
rise in the decade prior to 2020 seems to have been followed by a sharp rise, and numbers have
stayed high ever since. We do not have the equivalent data for adults, meaning that a clear picture
has yet to emerge, but there is persuasive evidence that levels of mental ill health have been rising
over the last decade, and the pandemic has contributed to many of the risk factors people face.
Before concluding as follows:
Crucially, the pandemic exposed fault-lines in the nation’s mental health, and the stark inequalities
faced every day by people living with mental illness. The public’s mental health was deteriorating
in the years running up to the pandemic, and mental health services were struggling to deal with
the consequences of many years of underfunding and austerity measures across public services.
People with a mental illness were already dying 15-20 years sooner than the general population, and
facing widespread hardship. The pandemic exacerbated these inequalities, creating new risks to
people’s mental health and reducing access to support.
We now have the opportunity to learn from this experience and build a mentally healthier future.
We can act now to boost the public’s mental health in the aftermath of the pandemic, protecting
those who have experienced the worst effects and offering better support to groups that don’t yet
have access to the right support. And we can incorporate mental health into preparations for future
emergencies, so that responses are psychologically informed from day one.
They also made 10 recommendations, mostly for the NHS and Department for Health and Care, but also covering education, communications and considerations for the upcoming (at the time) review of the Mental Health Act. Less than half of these recommendations have been addressed at all.
Now we are two years on from that report, what has changed?
Well, Roy Lilley has drawn a rather dispiriting picture for us. He draws attention to Wes Streeting’s announcement in the Health Service Journal on 12 March, that the proportion of the NHS budget spent on mental healthcare would be cut for the third year in a row. Lilley lists how the demands on mental health services have mushroomed since before the pandemic:
- Around two million people were in touch with mental health services in 2019, today it’s around three million;
- Child and Adolescent Services: in 2019 around 500,000 referrals. Now around a million;
- And only around 45% of referrals are accepted, meaning the true demand is even higher;
- Talking therapies are up by 60%; and
- Crisis team referrals and sectioning under the Mental Health Act are also up 60%.
And he summarises the problem like this:
The total economic cost of mental ill-health in England in 2022 was estimated ~£300bn a year when lost productivity, welfare and wider costs are factored in.
The total MH budget is about £16bn. Meaning, the NHS is spending roughly £1 trying to address a £18 national problem.
It feels like we are still waiting for the penny to drop.
